Understanding Functional Neurological Disorder
A conceptual understanding of Functional Neurological Disorder
By Dr. David Traster, DC, MS, DACNB
Co-owner, The Neurologic Wellness Institute
Boca Raton • Chicago • Waukesha • Wood Dale
www.neurologicwellnessinstitute.com
The Patient Who Couldn’t Walk—But Had Nothing “Wrong”
He sat across from me, frustrated and exhausted. His leg would give out without warning. Some days he could walk normally. Other days, he couldn’t trust his body at all. He had been through MRIs, blood work, neurological exams—everything was “normal.”
And yet, nothing about his experience felt normal.
This is where many patients fall into a gap in medicine. When we don’t see structural damage—no stroke, no tumor, no nerve injury—the assumption has historically been that nothing is wrong. But modern neuroscience is telling us something very different.
Sometimes, the problem is not in the structure of the brain.
It’s in how the brain is functioning.
A Brain That Predicts, Not Just Reacts
For most of medical history, we’ve thought of the brain as a reactive organ—something that responds to the world as it happens. But that’s not how it actually works.
The brain is constantly predicting.
It builds models of what it expects to feel, see, and do. It anticipates movement before it happens. It predicts sensory input before it arrives. This process—often called predictive processing—is how we move smoothly, maintain balance, and interact with the world without having to consciously think about every action.
Under normal conditions, these predictions are continuously updated by incoming sensory information. The brain makes a prediction, compares it to reality, and adjusts.
But what happens when that system becomes imbalanced?
When Predictions Override Reality
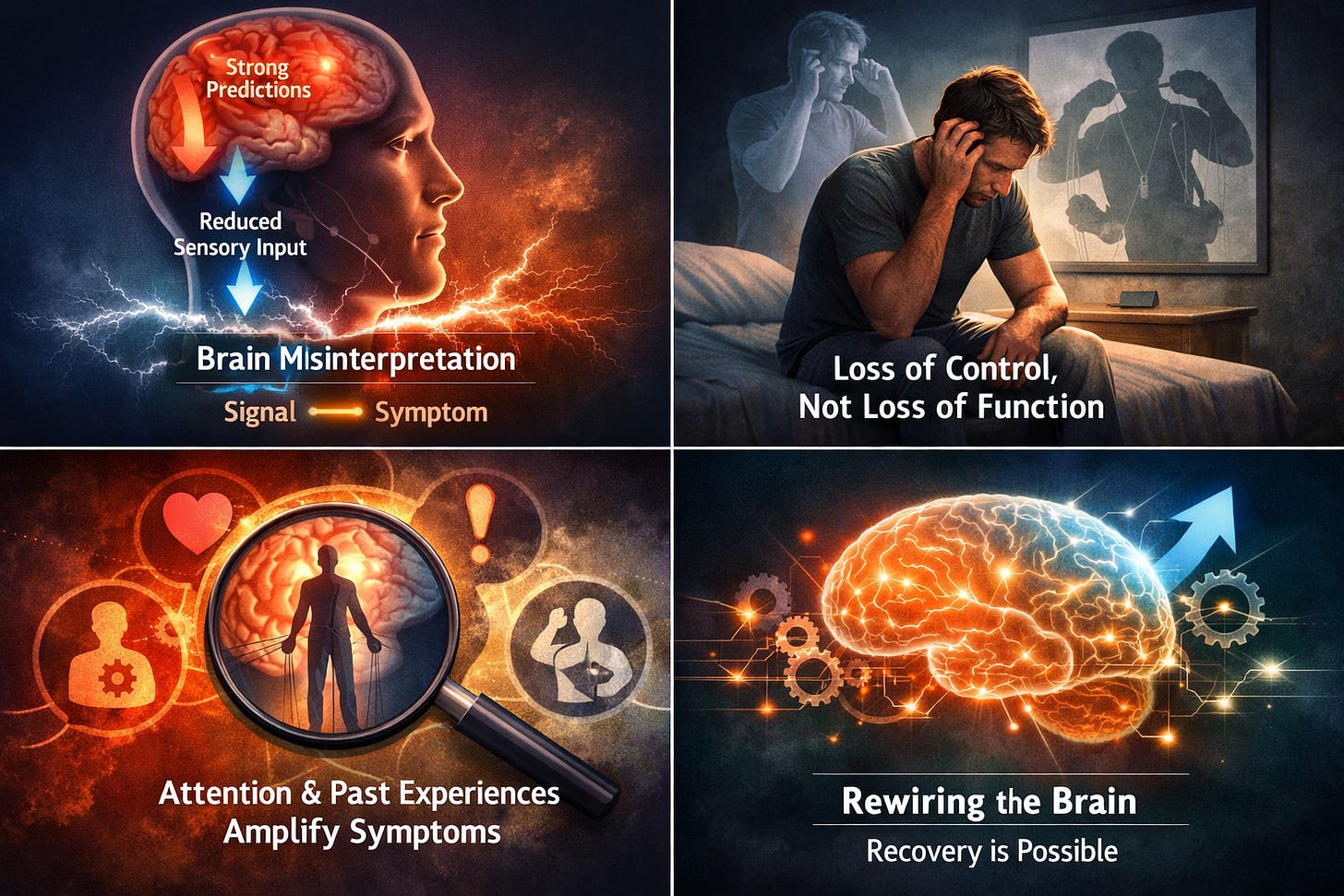
In Functional Neurological Disorder (FND), the brain begins to rely too heavily on its predictions—and not enough on actual sensory input.
The result is profound.
The brain can generate symptoms—real symptoms—that feel exactly like neurological disease. Weakness. Tremors. Dizziness. Loss of control. Even seizures.
But these symptoms are not coming from damaged tissue.
They are coming from a mismatch between what the brain expects and what the body is actually doing.
It’s not imagined. It’s not voluntary.
It is a brain-based problem of signal processing.
Attention: The Amplifier of Symptoms
One of the most powerful drivers of this process is attention.
Where attention goes, brain activity follows.
In FND, attention becomes overly focused on the body. Normal sensations—subtle shifts in balance, muscle tension, internal signals—become magnified. The brain assigns too much importance to these signals, increasing their “precision.”
This creates a feedback loop.
The more attention is directed toward a symptom, the stronger the brain’s prediction becomes. The stronger the prediction, the more real the symptom feels.
Over time, this loop can become self-sustaining.
The Loss of Control Without Loss of Function
One of the most confusing aspects of FND—for both patients and clinicians—is this paradox:
The system works… but the patient can’t access it.
A patient with functional leg weakness may not be able to voluntarily move their leg during an exam. But when distracted, or in a different context, the movement may return.
This tells us something critical.
The motor pathways are intact.
The problem is not the ability to move—it’s the brain’s ability to access and control that movement in a predictable way.
This is why symptoms often fluctuate, disappear with distraction, or change over time. The underlying system is still there. It’s just not being used correctly.
The Brain Networks Behind the Symptoms
Functional Neurological Disorder is not localized to a single region of the brain. Instead, it involves a network-level disruption.
Motor areas responsible for movement.
Sensory regions processing incoming information.
The limbic system, which assigns emotional significance.
The prefrontal cortex, where beliefs and expectations are formed.
And the salience network, which decides what matters and what doesn’t.
When these systems become misaligned, the brain can generate outputs that feel completely real—but are not being guided by accurate sensory input.
Why Past Experience Matters
The brain does not create predictions in a vacuum.
It builds them from past experience.
Previous injuries. Illnesses. Emotional stress. Repeated attention to symptoms. Even things a patient has been told about their body.
Over time, these experiences shape the brain’s expectations.
If the brain learns that a certain movement is dangerous, unstable, or associated with discomfort, it may begin to predict failure—even in the absence of any structural problem.
And once that prediction becomes strong enough, the body follows.
Why the Symptoms Feel So Real
This is one of the most important points to understand.
The symptoms in FND are not fake.
They are generated by the same brain systems that produce all movement, sensation, and perception. The difference is that the signals are being driven by faulty predictions rather than accurate sensory integration.
To the patient, the experience is indistinguishable from structural disease.
Because from the brain’s perspective, it is real.
Diagnosis: Finding What’s There, Not Just What’s Missing
For years, FND was considered a diagnosis of exclusion—something you arrived at only after ruling everything else out.
That approach is outdated.
We now recognize that FND can be diagnosed based on positive clinical signs.
Movements that improve with distraction.
Weakness that doesn’t follow anatomical patterns.
Symptoms that are internally inconsistent.
These findings are not vague—they are specific indicators of how the brain is functioning.
And recognizing them early matters.
The Most Powerful First Treatment: Understanding
One of the most effective interventions in FND is also the simplest.
Explanation.
When patients understand that their symptoms are coming from the brain—but not from damage—it changes everything.
It shifts the narrative from “something is broken” to “something can be retrained.”
This alone can begin to reduce symptom intensity.
Because it changes the brain’s expectations.
Rewiring the System
If FND is a problem of prediction, attention, and control, then treatment must target those same systems.
Movement retraining.
Vestibular and sensory integration.
Attention redirection.
Cognitive reframing.
Gradual exposure to previously avoided movements.
These approaches work not by forcing the body, but by updating the brain’s internal model.
Over time, the brain relearns what is safe, what is stable, and what is possible.
And the symptoms begin to fade.
The Brain That Can Change
The most important takeaway is this:
Functional Neurological Disorder is not a dead end.
It is a dynamic, reversible condition rooted in the brain’s ability to learn—and, importantly, to relearn.
The same neuroplasticity that allowed the symptoms to develop is the mechanism through which they can resolve.
The brain that created the problem is also the brain that can fix it.
And for many patients, that realization is the beginning of recovery.
REFERENCES
Edwards MJ, Adams RA, Brown H, Pareés I, Friston KJ. A Bayesian account of ‘hysteria.’ Brain. 2012;135(11):3495–3512.
Hallett M. Functional (psychogenic) movement disorders—Clinical presentations. Parkinsonism Relat Disord. 2016;22(Suppl 1):S149–S152.
Perez DL, Edwards MJ, Nielsen G, Kozlowska K, Hallett M, LaFrance WC Jr. Decade of progress in motor functional neurological disorder: Continuing the momentum. J Neurol Neurosurg Psychiatry. 2021;92(6):668–677.
Stone J, Carson A, Duncan R, et al. Who is referred to neurology clinics?—The diagnoses made in 3781 new patients. Clin Neurol Neurosurg. 2010;112(9):747–751.
Voon V, Cavanna AE, Coburn K, et al. Functional neuroanatomy and neurophysiology of functional neurological disorders (conversion disorder). J Neuropsychiatry Clin Neurosci. 2016;28(3):168–190.
Teodoro T, Edwards MJ, Isaacs JD. A unifying theory for cognitive abnormalities in functional neurological disorders, fibromyalgia, and chronic fatigue syndrome: Systematic review. J Neurol Neurosurg Psychiatry. 2018;89(12):1308–1319.
Brown H, Adams RA, Pareés I, Edwards M, Friston K. Active inference, sensory attenuation, and illusions. Cogn Process. 2013;14(4):411–427.
Pick S, Goldstein LH, Perez DL, Nicholson TR. Emotional processing in functional neurological disorder: A review, biopsychosocial model, and research agenda. J Neurol Neurosurg Psychiatry. 2019;90(6):704–711.
Gelauff JM, Stone J, Edwards MJ, Carson A. The prognosis of functional (psychogenic) motor symptoms: A systematic review. J Neurol Neurosurg Psychiatry. 2014;85(2):220–226.
Aybek S, Perez DL. Diagnosis and management of functional neurological disorder. BMJ. 2022;376:o64.


Thank you. FND is something that's very hard to understand if you haven't experienced it yourself. The simplest tasks--walking, picking up a pencil--can suddenly take as much focus as walking a tightrope. And a moment later-- back to normal. I questioned my own sanity.
During my most recent bout, I saw a neurological physical therapist. After 3 months of hard work, I went from barely shuffling to hiking mountains. I still "glitch" when I'm overtired, but have learned to manage my remaining symptoms.
My Substack details my personal experience, the latest research findings, and why the diagnosis is still so misunderstood. https://drsullins.substack.com/
Excellent article. Could the brain's prediction and anticipation of disfluency and the resulting anticipation and anxiety associated with stuttering, actually cause the stutter?
If not, why not? It seems to follow the same pattern based on this excellent article?